Vacuum-Assisted Core Biopsy
What are the prerequisites for having a vacuum-assisted core biopsy done? Recent previous imaging that has identified an abnormality requiring…
Read more
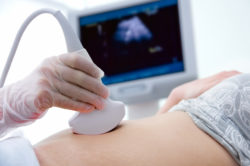
Figure 1: Image of an ultrasound examination
Chorionic villous sampling (CVS) is offered from week 11 of pregnancy to women who are at a high risk of their foetus (unborn baby) being born with Down syndrome, or other chromosomal or inherited conditions. CVS also confirms the sex of the foetus, which can be important in identifying X-chromosome (female) linked inherited conditions. CVS is best carried out between week 11 and week 13 of a pregnancy.
A needle is inserted into the abdomen just below the navel (belly button) to take a small sample of tissue from the placenta (the organ that develops inside the uterus (womb) to supply food and oxygen to the foetus). CVS uses ultrasound images (or pictures) to guide the needle into the placenta (see: Ultrasound).
The sample of tissue is tested to detect any genetic conditions that can sometimes be inherited.
CVS is the most effective way to detect those chromosomal or genetic conditions for which testing is currently possible.
There is a similar test called amniocentesis that is also used to test for chromosomal and some inherited conditions. This can be carried out later in pregnancy if required (see: Amniocentesis).
Women are referred for CVS if they receive a high-risk result from screening carried out in the first trimester of pregnancy (see Nuchal Translucency Scan) if it shows a likelihood of the foetus having Down Syndrome or other chromosomal conditions. CVS gives a definite diagnosis that will help to guide the discussion between you and your doctor about your pregnancy.
Other reasons your doctor would recommend CVS might be:
Before having CVS, you will need to know your blood group. If you or your doctor do not know your blood group, then a blood test should be arranged by the doctor who is referring you for CVS. Your blood group needs to be identified to see whether, within your blood group, you are Rhesus positive or Rhesus negative. If you have a different blood type from your foetus and you have Rhesus negative blood, you might form antibodies. This can cause the foetus to have an illness, such as low blood count, which can range from mild to severe.
To avoid this, Rhesus negative women will need to be immunised by having a small injection of anti-D after the procedure. This will prevent your body forming these antibodies against the foetus and against any future pregnancies. Your doctor will talk to you about this and arrange any necessary immunisation.
You should have some fluid in your bladder, but not be uncomfortably full. This is to ensure that the inside of the abdomen is seen clearly on the ultrasound images when the needle is being guided into place. The facility where you are having the test will provide information about this. No further preparation is needed.
The specialist doctor carrying out the CVS will fully explain the procedure, and inform you of the risks and reasons for having the test. You will usually be given a consent form to read and sign. You might have already discussed the test, the reasons you have been referred for a CVS, and the benefits and risks with a genetic counsellor. If you have any questions, feel free to ask your own doctor, the counsellor or the specialist doctor before the procedure begins.
You will be asked to lie on an examination table. Gel is applied to the lower abdomen area, and a transducer (a smooth hand held device) is moved gently across the abdomen with a sliding and rotating action. The transducer transmits ultrasound waves that are relayed back to the ultrasound machine to produce images onto an ultrasound screen (see Ultrasound).
The ultrasound is carried out before having the CVS to check previous ultrasound findings and confirm they are correct. It will confirm the age of the foetus, the position of the placenta and look at the anatomy or structure of the foetus for any signs of abnormality.
The ultrasound will also allow the doctor to assess where the safest position is to insert the needle for the CVS.
The skin is cleaned with antiseptic solution, and you would usually be given an injection of local anaesthetic to numb your skin and the deeper layers of your abdomen where the needle taking the sample will be inserted.
The CVS needle is then gently inserted into your abdomen just below the navel, using ultrasound images for guidance. The images you see on the screen show what is happening inside your body at that moment like a movie. This allows the doctor to guide the needle as it is inserted through the lower abdominal wall and uterus, and then into its correct position in the placenta well away from the foetus.
The discomfort when the needle is inserted is fairly minimal and lasts a few seconds.
The CVS needle is inserted once, and a smaller inner needle is inserted through the middle of the CVS needle and takes a small sample of tissue (a ‘biopsy’) from the placenta. It might be necessary to take more than one biopsy sample using this inner needle to ensure there is enough tissue for testing. You should not feel the samples being taken. The amount of tissue required for testing is very small, about the size of a small grain of rice. It is important that you remain still while the needle is being inserted and the sample is taken, so that the needle can be accurately positioned and clearly seen on the ultrasound images by the doctor carrying out the test. During the procedure, you might feel discomfort or a ‘dragging’ type feeling in your lower abdomen. It is recommended you arrange for someone to drive you to the radiology facility where you are having the test and drive you home after the procedure. When home, rest for a couple of hours in bed or on a couch. You can do normal (non-strenuous) activities at home for the rest of the day, but avoid any strenuous exercise or lifting.
You might experience crampy period-like pain, but this normally settles with paracetamol or other non-prescription painkillers, which are safe for you to take. Avoid the use of aspirin, as this might lead to possible bleeding. If you are unsure whether your painkillers are safe for you take, please ask the doctor doing the test or your own doctor.
You might also experience slight vaginal bleeding, which should settle in 24–36 hours. If you have a large amount of vaginal bleeding; for example, fresh red blood like a period bleed, or bleeding continues for more than 36 hours, you should contact the facility where the procedure was carried out or see your doctor (or the nearest hospital emergency department if this occurs on a weekend or at night).
The whole procedure usually takes approximately 30 minutes. This includes the initial ultrasound examination, preparing your skin with antiseptic and local anaesthetic, and finding the best place to insert the CVS needle. Inserting the CVS needle and taking tissue samples takes only a few minutes.
CVS is invasive, because a needle is inserted into the placenta that is inside the uterus. The main risk is miscarriage.
There is a 1% risk of miscarriage. On average, 1 in 100 patients will miscarry and lose the pregnancy. This is why the procedure is offered to women who have a higher than average risk of genetic or chromosomal abnormalities (See above: Why would my doctor refer me for CVS?).
There is a small risk of infection. If you have symptoms of fever, chills or are leaking fluid from your vagina after the procedure, you should see your doctor (or the nearest hospital emergency department if this occurs on a weekend or at night).
Although CVS is able to identify Down syndrome, chromosomal, genetic or inherited conditions, there are some chromosomal and genetic disorders for which there are currently no tests available.
The benefit of CVS is to allow doctors to confidently confirm if the foetus does or does not have Down syndrome, or a wide variety of other chromosomal and also some genetic abnormalities.
CVS can also determine some inherited conditions, such as cystic fibrosis, and determine the paternity (the identity of the father) of the foetus if required.
You will need to consider the benefits of the test, such as finding out if a foetus has abnormalities, against the risks of miscarriage. If you do not have the test, you might not know about these abnormalities until much later in the pregnancy or after the baby is born. If you are unsure about having the test, then discuss this with your specialist or genetic councillor.
The test is always carried out by a specialist doctor, either a radiologist or more commonly an obstetrician/ultrasonologist who has had additional training in this area of obstetric and foetal ultrasound.
CVS is carried out in a radiology or other hospital department, a private practice or at a specialist clinic for obstetric and gynaecological imaging. All facilities will have appropriately trained staff to carry out the procedure. The ultrasound room is usually dimly lit to allow the images on the ultrasound screen to be clearly seen.
The tissue sample (biopsy) from the placenta is sent to a special laboratory that will carry out a number of tests. The tissue sample is placed in culture medium and allowed to grow in a warm incubator for 7–10 days, and then examined for chromosomes that might indicate an abnormality. There are 23 pairs of chromosomes, all of which are examined in detail. This process takes approximately 10–14 days, after which the results are available to your doctor.
A written report will be sent to your referring doctor, and you will generally need to go back to your referring doctor or specialist clinic for the results of the test.
Some specialist centres might offer a rapid result (an interim report) in 24 hours (called a FISH test).
The National Health and Medical Research Council (NHMRC) www.nhmrc.gov.au
Page last modified on 18/8/2017.
RANZCR® is not aware that any person intends to act or rely upon the opinions, advices or information contained in this publication or of the manner in which it might be possible to do so. It issues no invitation to any person to act or rely upon such opinions, advices or information or any of them and it accepts no responsibility for any of them.
RANZCR® intends by this statement to exclude liability for any such opinions, advices or information. The content of this publication is not intended as a substitute for medical advice. It is designed to support, not replace, the relationship that exists between a patient and his/her doctor. Some of the tests and procedures included in this publication may not be available at all radiology providers.
RANZCR® recommends that any specific questions regarding any procedure be discussed with a person's family doctor or medical specialist. Whilst every effort is made to ensure the accuracy of the information contained in this publication, RANZCR®, its Board, officers and employees assume no responsibility for its content, use, or interpretation. Each person should rely on their own inquires before making decisions that touch their own interests.